Search
- Page Path
- HOME > Search
- Adrenal gland
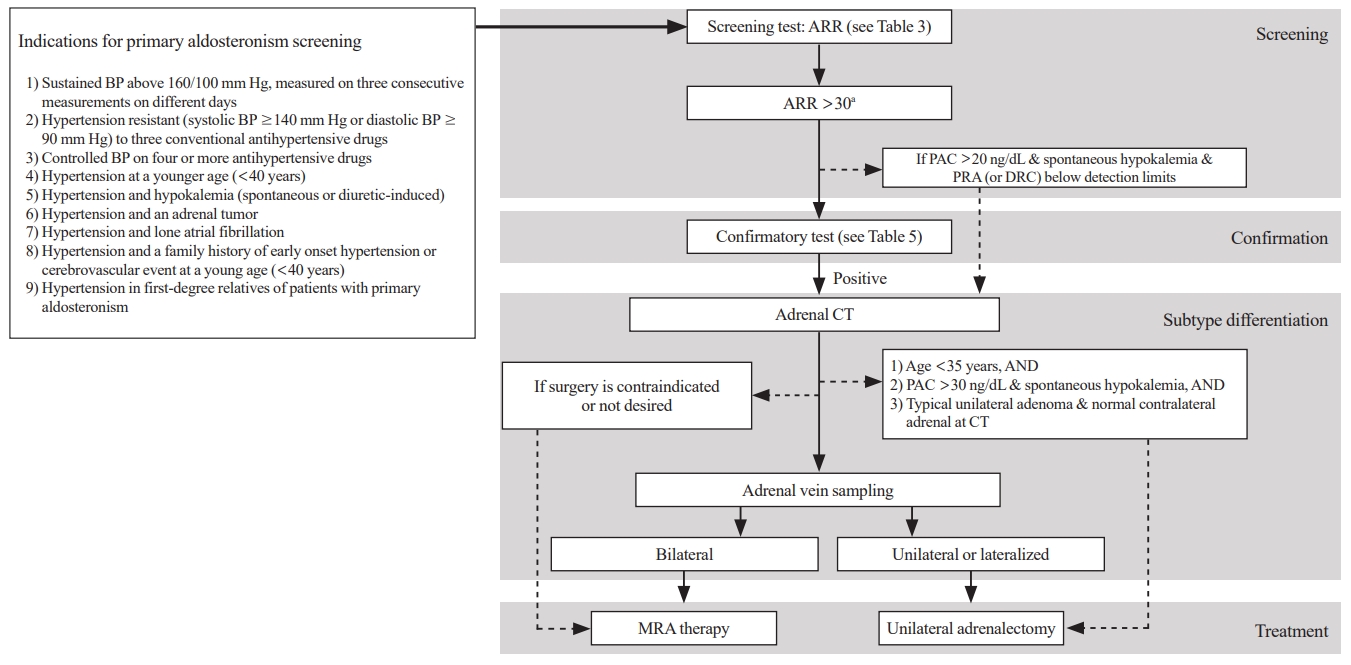
- 2023 Korean Endocrine Society Consensus Guidelines for the Diagnosis and Management of Primary Aldosteronism
- Jeonghoon Ha, Jung Hwan Park, Kyoung Jin Kim, Jung Hee Kim, Kyong Yeun Jung, Jeongmin Lee, Jong Han Choi, Seung Hun Lee, Namki Hong, Jung Soo Lim, Byung Kwan Park, Jung-Han Kim, Kyeong Cheon Jung, Jooyoung Cho, Mi-kyung Kim, Choon Hee Chung, The Committee of Clinical Practice Guideline of Korean Endocrine Society, The Korean Adrenal Study Group of Korean Endocrine Society
- Endocrinol Metab. 2023;38(6):597-618. Published online October 13, 2023
- DOI: https://doi.org/10.3803/EnM.2023.1789
- 3,481 View
- 484 Download
- 1 Web of Science
- 1 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub - Primary aldosteronism (PA) is a common, yet underdiagnosed cause of secondary hypertension. It is characterized by an overproduction of aldosterone, leading to hypertension and/or hypokalemia. Despite affecting between 5.9% and 34% of patients with hypertension, PA is frequently missed due to a lack of clinical awareness and systematic screening, which can result in significant cardiovascular complications. To address this, medical societies have developed clinical practice guidelines to improve the management of hypertension and PA. The Korean Endocrine Society, drawing on a wealth of research, has formulated new guidelines for PA. A task force has been established to prepare PA guidelines, which encompass epidemiology, pathophysiology, clinical presentation, diagnosis, treatment, and follow-up care. The Korean clinical guidelines for PA aim to deliver an evidence-based protocol for PA diagnosis, treatment, and patient monitoring. These guidelines are anticipated to ease the burden of this potentially curable condition.
-
Citations
Citations to this article as recorded by- Correlation of Histopathologic Subtypes of Primary Aldosteronism with Clinical Phenotypes and Postsurgical Outcomes
Chang Ho Ahn, You-Bin Lee, Jae Hyeon Kim, Young Lyun Oh, Jung Hee Kim, Kyeong Cheon Jung
The Journal of Clinical Endocrinology & Metabolism.2023;[Epub] CrossRef
- Correlation of Histopathologic Subtypes of Primary Aldosteronism with Clinical Phenotypes and Postsurgical Outcomes

- Miscellaneous
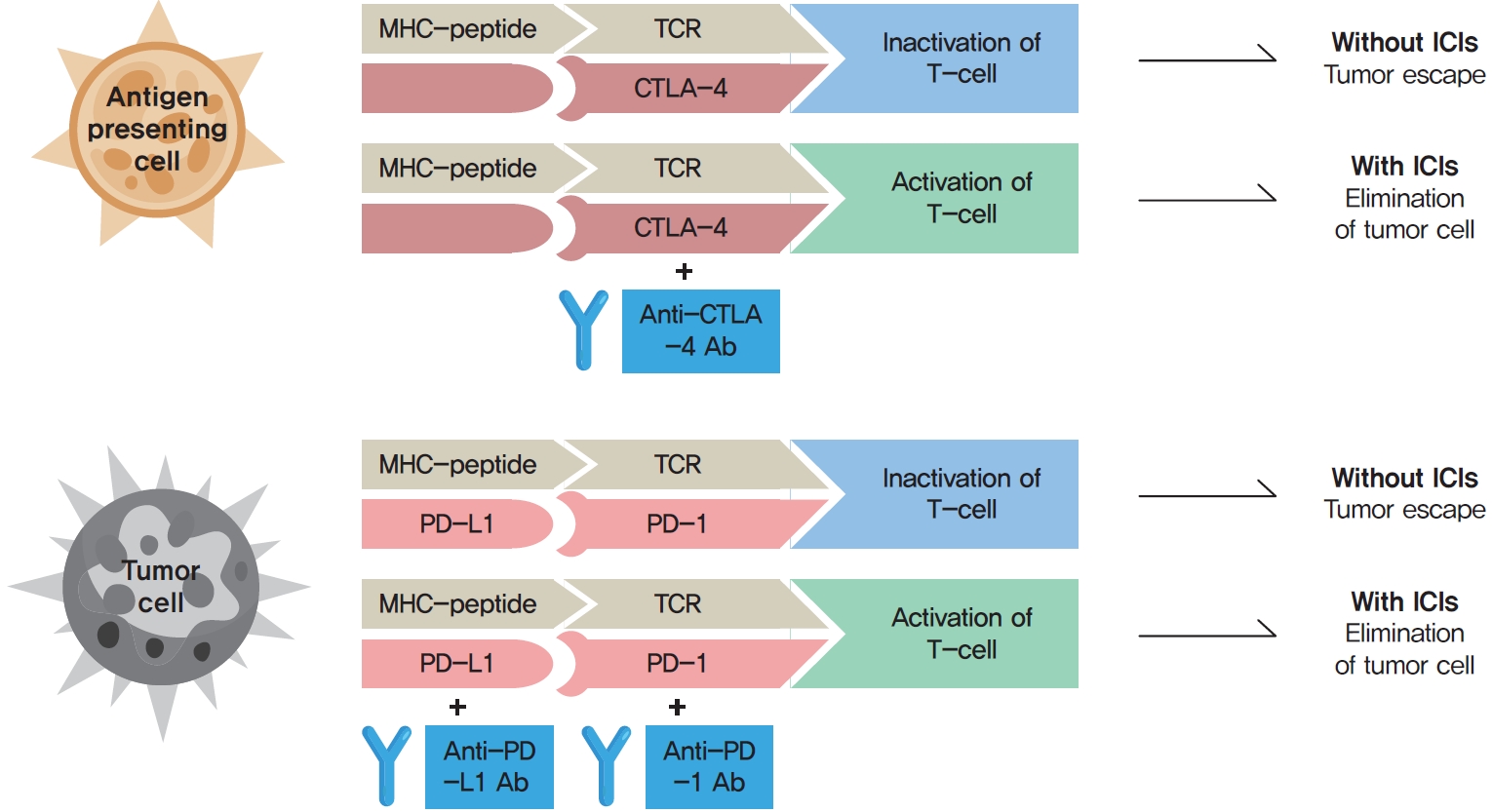
- Immune Checkpoint Inhibitors and Endocrine Disorders: A Position Statement from the Korean Endocrine Society
- Hyemi Kwon, Eun Roh, Chang Ho Ahn, Hee Kyung Kim, Cheol Ryong Ku, Kyong Yeun Jung, Ju Hee Lee, Eun Heui Kim, Sunghwan Suh, Sangmo Hong, Jeonghoon Ha, Jun Sung Moon, Jin Hwa Kim, Mi-kyung Kim, The Committee of Clinical Practice Guideline of the Korean Endocrine Society
- Endocrinol Metab. 2022;37(6):839-850. Published online December 26, 2022
- DOI: https://doi.org/10.3803/EnM.2022.1627
- 3,516 View
- 321 Download
- 2 Web of Science
- 2 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub - Immune checkpoint inhibitors (ICIs) including an anti-cytotoxic T-lymphocyte-associated antigen 4 inhibitor, anti-programmed cell death protein 1 (PD-1) inhibitors, and anti-PD-ligand 1 inhibitors are representative therapeutics for various malignancies. In oncology, the application of ICIs is currently expanding to a wider range of malignancies due to their remarkable clinical outcomes. ICIs target immune checkpoints which suppress the activity of T-cells that are specific for tumor antigens, thereby allowing tumor cells to escape the immune response. However, immune checkpoints also play a crucial role in preventing autoimmune reactions. Therefore, ICIs targeting immune checkpoints can trigger various immune-related adverse events (irAEs), especially in endocrine organs. Considering the endocrine organs that are frequently involved, irAEs associated endocrinopathies are frequently life-threatening and have unfavorable clinical implications for patients. However, there are very limited data from large clinical trials that would inform the development of clinical guidelines for patients with irAEs associated endocrinopathies. Considering the current clinical situation, in which the scope and scale of the application of ICIs are increasing, position statements from clinical specialists play an essential role in providing the appropriate recommendations based on both medical evidence and clinical experience. As endocrinologists, we would like to present precautions and recommendations for the management of immune-related endocrine disorders, especially those involving the adrenal, thyroid, and pituitary glands caused by ICIs.
-
Citations
Citations to this article as recorded by- Pembrolizumab plus lenvatinib for radically unresectable or metastatic renal cell carcinoma in the Japanese population
Ryo Fujiwara, Takeshi yuasa, kenichi kobayashi, tetsuya yoshida, susumu kageyama
Expert Review of Anticancer Therapy.2023; 23(5): 461. CrossRef - Incidence of Endocrine-Related Dysfunction in Patients Treated with New Immune Checkpoint Inhibitors: A Meta-Analysis and Comprehensive Review
Won Sang Yoo, Eu Jeong Ku, Eun Kyung Lee, Hwa Young Ahn
Endocrinology and Metabolism.2023; 38(6): 750. CrossRef
- Pembrolizumab plus lenvatinib for radically unresectable or metastatic renal cell carcinoma in the Japanese population

- Miscellaneous
- COVID-19 Vaccination for Endocrine Patients: A Position Statement from the Korean Endocrine Society
- Cheol Ryong Ku, Kyong Yeun Jung, Chang Ho Ahn, Jun Sung Moon, Ju Hee Lee, Eun Heui Kim, Hyemi Kwon, Hee Kyung Kim, Sunghwan Suh, Sangmo Hong, Jeonghoon Ha, Eun Roh, Jin Hwa Kim, Mi-kyung Kim, the Committee of Clinical Practice Guideline of the Korean Endocrine Society
- Endocrinol Metab. 2021;36(4):757-765. Published online August 17, 2021
- DOI: https://doi.org/10.3803/EnM.2021.404
- 10,377 View
- 419 Download
- 19 Web of Science
- 21 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub - Since the first outbreak of coronavirus disease 2019 (COVID-19), ongoing efforts have been made to discover an efficacious vaccine against COVID-19 to combat the pandemic. In most countries, both mRNA and DNA vaccines have been administered, and their side effects have also been reported. The clinical course of COVID-19 and the effects of vaccination against COVID-19 are both influenced by patients’ health status and involve a systemic physiological response. In view of the systemic function of endocrine hormones, endocrine disorders themselves and the therapeutics used to treat them can influence the outcomes of vaccination for COVID-19. However, there are very limited data to support the development of clinical guidelines for patients with specific medical backgrounds based on large clinical trials. In the current severe circumstances of the COVID-19 pandemic, position statements made by clinical specialists are essential to provide appropriate recommendations based on both medical evidence and clinical experiences. As endocrinologists, we would like to present the medical background of COVID-19 vaccination, as well as precautions to prevent the side effects of COVID-19 vaccination in patients with specific endocrine disorders, including adrenal insufficiency, diabetes mellitus, osteoporosis, autoimmune thyroid disease, hypogonadism, and pituitary disorders.
-
Citations
Citations to this article as recorded by- COVID-19 mRNA vaccine may trigger subacute thyroiditis
Mehmet Sözen, Ömercan Topaloğlu, Berrin Çetinarslan, Alev Selek, Zeynep Cantürk, Emre Gezer, Damla Köksalan, Taner Bayraktaroğlu
Human Vaccines & Immunotherapeutics.2024; 17(12): 5120. CrossRef - The role of co-morbidities in the development of an AEFI after COVID-19 vaccination in a large prospective cohort with patient-reported outcomes in the Netherlands
C. Ouaddouh, J.W. Duijster, T. Lieber, F.P.A.M. van Hunsel
Expert Opinion on Drug Safety.2024; 23(3): 323. CrossRef - Thyroid dysfunction in COVID-19
David Tak Wai Lui, Chi Ho Lee, Yu Cho Woo, Ivan Fan Ngai Hung, Karen Siu Ling Lam
Nature Reviews Endocrinology.2024;[Epub] CrossRef - Adult-Onset Type 1 Diabetes Development Following COVID-19 mRNA Vaccination
Hyeyeon Moon, Sunghwan Suh, Mi Kyoung Park
Journal of Korean Medical Science.2023;[Epub] CrossRef - Prior immunization status of COVID-19 patients and disease severity: A multicenter retrospective cohort study assessing the different types of immunity
Javaria Aslam, Faisal Shahzad Khan, Muhammad Talha Haris, Hewad Hewadmal, Maryam Khalid, Mohammad Y. Alshahrani, Qurrat-ul-ain Aslam, Irrum Aneela, Urooj Zafar
Vaccine.2023; 41(2): 598. CrossRef - Mortality and Severity of Coronavirus Disease 2019 in Patients with Long-Term Glucocorticoid Therapy: A Korean Nationwide Cohort Study
Eu Jeong Ku, Keeho Song, Kyoung Min Kim, Gi Hyeon Seo, Soon Jib Yoo
Endocrinology and Metabolism.2023; 38(2): 253. CrossRef - Pituitary Diseases and COVID-19 Outcomes in South Korea: A Nationwide Cohort Study
Jeonghoon Ha, Kyoung Min Kim, Dong-Jun Lim, Keeho Song, Gi Hyeon Seo
Journal of Clinical Medicine.2023; 12(14): 4799. CrossRef - Inactivated SARS-CoV-2 vaccination does not disturb the clinical course of Graves’ disease: An observational cohort study
Shichen Xu, Huixin Yu, Xian Cheng, Jing Wu, Jiandong Bao, Li Zhang
Vaccine.2023; 41(38): 5648. CrossRef - Adrenal Crisis Associated With COVID-19 Vaccination in Patients With Adrenal Insufficiency
Yukako Kurematsu, Takako Mohri, Sadanori Okada, Yutaka Takahashi
JCEM Case Reports.2023;[Epub] CrossRef - Adverse Events Associated with COVID-19 Vaccination in Adolescents with Endocrinological Disorders: A Cross-Sectional Study
İbrahim Mert Erbaş, İrem Ceren Erbaş, Gözde Akın Kağızmanlı, Kübra Yüksek Acinikli, Özge Besci, Korcan Demir, Ece Böber, Nurşen Belet, Ayhan Abacı
Journal of Clinical Research in Pediatric Endocrinology.2023; 15(3): 248. CrossRef - Neue Aspekte der Glukokortikoidsubstitution bei Nebennierenrindeninsuffizienz
Tina Kienitz, Gesine Meyer
Der Internist.2022; 63(1): 12. CrossRef - Endocrine Follow-up During Post-Acute COVID-19: Practical Recommendations Based on Available Clinical Evidence
Rimesh Pal, Ameya Joshi, Sanjay K. Bhadada, Mainak Banerjee, Suresh Vaikkakara, Satinath Mukhopadhyay
Endocrine Practice.2022; 28(4): 425. CrossRef - Safety of Inactivated and mRNA COVID-19 Vaccination Among Patients Treated for Hypothyroidism: A Population-Based Cohort Study
Xi Xiong, Carlos King Ho Wong, Ivan Chi Ho Au, Francisco Tsz Tsun Lai, Xue Li, Eric Yuk Fai Wan, Celine Sze Ling Chui, Esther Wai Yin Chan, Franco Wing Tak Cheng, Kristy Tsz Kwan Lau, Chi Ho Lee, Yu Cho Woo, David Tak Wai Lui, Ian Chi Kei Wong
Thyroid.2022; 32(5): 505. CrossRef - The New Entity of Subacute Thyroiditis amid the COVID-19 Pandemic: From Infection to Vaccine
Mihaela Popescu, Adina Ghemigian, Corina Maria Vasile, Andrei Costache, Mara Carsote, Alice Elena Ghenea
Diagnostics.2022; 12(4): 960. CrossRef - Adrenal Crisis Secondary to COVID-19 Vaccination in a Patient With Hypopituitarism
Nikolina Markovic, Anila Faizan, Chirag Boradia, Sridhar Nambi
AACE Clinical Case Reports.2022; 8(4): 171. CrossRef - The Effect of Inactivated SARS-CoV-2 Vaccines on TRAB in Graves’ Disease
LingHong Huang, ZhengRong Jiang, JingXiong Zhou, YuPing Chen, HuiBin Huang
Frontiers in Endocrinology.2022;[Epub] CrossRef - Osteoporosis in Patients With Respiratory Diseases
Yue Ma, Shui Qiu, Renyi Zhou
Frontiers in Physiology.2022;[Epub] CrossRef - Pilot Findings on SARS-CoV-2 Vaccine-Induced Pituitary Diseases: A Mini Review from Diagnosis to Pathophysiology
Ach Taieb, El Euch Mounira
Vaccines.2022; 10(12): 2004. CrossRef - Forty Years Together, New Leap Forward! The 40th Anniversary of the Korean Endocrine Society
Jong Chul Won, Ki-Hyun Baek
Endocrinology and Metabolism.2022; 37(6): 851. CrossRef - No need of glucocorticoid dose adjustment in patients with adrenal insufficiency before COVID-19 vaccine
Tania Pilli, Cristina Dalmiglio, Gilda Dalmazio, Alfonso Sagnella, Raffaella Forleo, Lucia Brilli, Fabio Maino, Cristina Ciuoli, Maria Grazia Castagna
European Journal of Endocrinology.2022; 187(1): K7. CrossRef - Diabetes and COVID-19 Vaccination
Hae Dong Choi, Jun Sung Moon
The Journal of Korean Diabetes.2021; 22(4): 221. CrossRef
- COVID-19 mRNA vaccine may trigger subacute thyroiditis

- Metabolic Surgery in Korea: What to Consider before Surgery
- Mi-Kyung Kim, Yoonseok Heo
- Endocrinol Metab. 2017;32(3):307-315. Published online September 18, 2017
- DOI: https://doi.org/10.3803/EnM.2017.32.3.307
- 4,302 View
- 48 Download
- 1 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Obesity is increasing globally and represents a significant global health problem because it predisposes towards various diseases, such as type 2 diabetes mellitus, cardiovascular disease, degenerative joint disease, and certain types of cancer. Numerous studies have shown that bariatric surgery reduces body mass and ameliorates obesity-related complications, such as hypertension and hyperglycemia, suggesting that surgery is the most effective therapeutic option for severely obese and obese diabetic patients. Recent international guidelines recommend surgical treatment for diabetic patients with class III obesity (body mass index [BMI] >40 kg/m2), regardless of their level of glycemic control or the complexity of their glucose-lowering regimens, and for patients with class II obesity (BMI 35.0 to 39.9 kg/m2) and hyperglycemia that is poorly controlled despite appropriate lifestyle and pharmacological therapy. The most popular procedures are Roux-en-Y gastric bypass and sleeve gastrectomy, but new procedures with better outcomes have been reported. For optimal surgical outcome, comprehensive management including assessments of a medical condition, nutrition, mental health, and social support is needed before and after surgery. However, there is still a lack of understanding regarding metabolic surgery in Korea. Therefore, this article reviews indications for metabolic surgery in patients with a specific focus on the situation in Korea.
-
Citations
Citations to this article as recorded by- Relationship between peak expiratory flow and impaired functional capacity in obese individuals
Graziele Mayra Santos Moreira, Angela Maria Ribeiro, Patrícia Maria de Melo Carvalho, Pedro Augusto de Carvalho Mira, Isabelle Magalhães Guedes Freitas
Fisioterapia em Movimento.2021;[Epub] CrossRef
- Relationship between peak expiratory flow and impaired functional capacity in obese individuals

- Clinical Characteristics of Patients with Adrenal Insufficiency in a General Hospital
- Ye Yeon Lee, Nan Hee Cho, Jong Won Lee, Nam Kyung Kim, Hye Soon Kim, Mi-Kyung Kim
- Endocrinol Metab. 2017;32(1):83-89. Published online February 28, 2017
- DOI: https://doi.org/10.3803/EnM.2017.32.1.83
- 4,462 View
- 60 Download
- 6 Web of Science
- 6 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Background Adrenal insufficiency (AI) is a life-threatening disorder caused by the deficiency of adrenal steroid hormones. This retrospective cross-sectional study investigated the characteristics of patients with AI in Korea.
Methods All consecutive patients with suspected AI who received care at a tertiary referral center in Korea in 2014 and underwent adrenocorticotropic hormone stimulation or insulin-tolerance testing were identified through a review of medical charts. Patients diagnosed with AI were enrolled. Their demographic, clinical, and treatment details were extracted.
Results Of 771 patients with suspected AI, 183 (23.7%) received a definitive diagnosis. The most common reason for testing was the presence of suspicious AI-related symptoms (30.0%), followed by a history of steroid medications (23.5%). Their mean age was 66.7 years, and females predominated (67.8%). The most common symptoms were general weakness, anorexia, arthralgia, and fever. Approximately half (53.6%) had a history of steroid use. Hydrocortisone was the most common treatment (71.6%), with most patients taking a 30 mg dose (44.2%). The most common dose frequency was twice a day (78.6%). Fourteen patients were treated for adrenal crisis (
n =10, 5.5%) or an intercurrent illness (n =4, 2.2%).Conclusion AI may have been caused by steroid medication use in many of the patients included in this study. The detection of AI can be improved by careful history-taking and being alert to the possibility that a patient has used steroids.
-
Citations
Citations to this article as recorded by- Risk of Mental Illnesses in Patients With Hypopituitarism: A Nationwide Population-Based Cohort Study
I-Hua Wei, Chih-Chia Huang
Psychiatry Investigation.2022; 19(6): 418. CrossRef - The Role of the Pharmacist in Optimizing Cancer Immunotherapy: A Retrospective Study of Nivolumab Adverse Events
Bradley D. Menz, Jacinta L. Johnson, Davina F. Gillard, William Chong, Michael B. Ward
Journal of Pharmacy Practice.2021; 34(3): 386. CrossRef - Clinical and biochemical factors to predict biochemical adrenal insufficiency in hospitalized patients with indeterminate cortisol levels: a retrospective study
Worapaka Manosroi, Natapong Kosachunhanan, Pichitchai Atthakomol
BMC Endocrine Disorders.2020;[Epub] CrossRef - Possible adrenal insufficiency among fatigue patients in a psychosomatic medical clinic
Sunao Matsubayashi, Nobuhiro Nakatake, Takeshi Hara
Endocrine Journal.2020; 67(1): 53. CrossRef - Encountering COVID-19 as Endocrinologists
Eun-Jung Rhee, Jung Hee Kim, Sun Joon Moon, Won-Young Lee
Endocrinology and Metabolism.2020; 35(2): 197. CrossRef - Glucocorticoid management of adrenal insufficiency in the United Kingdom: assessment using real-world data
Kamran Iqbal, Kate Halsby, Robert D Murray, Paul V Carroll, Robert Petermann
Endocrine Connections.2019; 8(1): 20. CrossRef
- Risk of Mental Illnesses in Patients With Hypopituitarism: A Nationwide Population-Based Cohort Study

- Co-Culture of α TC-6 Cells and β TC-1 Cells: Morphology and Function
- Sung Man Kim, Eun Ju Lee, Hye Sook Jung, Na Han, You Jeong Kim, Tae Kyoon Kim, Tae Nyun Kim, Min Jeong Kwon, Soon Hee Lee, Jeong Hyun Park, Byoung Doo Rhee, Mi-Kyung Kim
- Endocrinol Metab. 2015;30(1):92-97. Published online March 27, 2015
- DOI: https://doi.org/10.3803/EnM.2015.30.1.92
- 4,635 View
- 72 Download
- 4 Web of Science
- 3 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Background In vitro experiments using only β-cell lines instead of islets are limited because pancreatic islets are composed of four different types of endocrine cells. Several recent studies have focused on cellular interactions among these cell types, especially α- and β-cells. Because islet isolation needs time and experience, we tested a simple co-culture system with α- and β-cells. Their morphology and function were assessed by comparison to each single cell culture and pancreatic islets.Methods α TC-6 cells and β TC-1 cells were maintained in Dulbecco's Minimal Essential Medium containing 5 mM glucose and 10% fetal bovine serum. Cells were mixed at a 1:1 ratio (5×105) in 6-well plates and cultured for 24, 48, and 72 hours. After culture, cells were used for insulin and glucagon immunoassays and tested for glucose-stimulated insulin secretion (GSIS).
Results α TC-6 and β TC-1 cells became condensed by 24 hours and were more strongly compacted after 48 hours. β TC-1 cells showed both β-β and β-α cell contacts. GSIS increased with increasing glucose concentration in co-cultured cells, which showed lower secreted insulin levels than β TC-1 cells alone. The increase in the secreted insulin/insulin content ratio was significantly lower for co-cultured cells than for β-cells alone (
P =0.04). Compared to islets, the α-/β-cell co-culture showed a higher ratio of GSIS to insulin content, but the difference was not statistically significant (P =0.09).Conclusion α TC-6 and β TC-1 cells in the co-culture system showed cell-to-cell contacts and a similar stimulated insulin secretion pattern to islets. The co-culture system may be used to better mimic pancreatic islets in
in vitro assessments.-
Citations
Citations to this article as recorded by- Recent advances in the design of implantable insulin secreting heterocellular islet organoids
M. Birgul Akolpoglu, Yasemin Inceoglu, Ugur Bozuyuk, Ana Rita Sousa, Mariana B. Oliveira, João F. Mano, Seda Kizilel
Biomaterials.2021; 269: 120627. CrossRef - Pancreatic β Cells Inhibit Glucagon Secretion from α Cells: An In Vitro Demonstration of α–β Cell Interaction
Wenqian Gu, Camilla Christine Bundgaard Anker, Christine Bodelund Christiansen, Tilo Moede, Per-Olof Berggren, Kjeld Hermansen, Søren Gregersen, Per Bendix Jeppesen
Nutrients.2021; 13(7): 2281. CrossRef - The Role of Pancreatic Alpha Cells and Endothelial Cells in the Reduction of Oxidative Stress in Pseudoislets
Fredrik C. Wieland, Mireille M.J.P.E. Sthijns, Thomas Geuens, Clemens A. van Blitterswijk, Vanessa L.S. LaPointe
Frontiers in Bioengineering and Biotechnology.2021;[Epub] CrossRef
- Recent advances in the design of implantable insulin secreting heterocellular islet organoids

- Obesity and Metabolism
- Response: A1c Variability Can Predict Coronary Artery Disease in Patients with Type 2 Diabetes with Mean A1c Level Greater than 7 (Endocrinol Metab 2013;28:125-32, Eun Ju Lee et al.)
- Eun Ju Lee, Mi-Kyung Kim
- Endocrinol Metab. 2013;28(4):348-349. Published online December 12, 2013
- DOI: https://doi.org/10.3803/EnM.2013.28.4.348
- 2,618 View
- 23 Download

- Obesity and Metabolism
- A1c Variability Can Predict Coronary Artery Disease in Patients with Type 2 Diabetes with Mean A1c Levels Greater than 7
- Eun Ju Lee, You Jeong Kim, Tae Nyun Kim, Tae Ik Kim, Won Kee Lee, Mi-Kyung Kim, Jeong Hyun Park, Byoung Doo Rhee
- Endocrinol Metab. 2013;28(2):125-132. Published online June 18, 2013
- DOI: https://doi.org/10.3803/EnM.2013.28.2.125
- 3,698 View
- 28 Download
- 12 Web of Science
- 15 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Background Recent studies suggested that the association of acute glucose variability and diabetic complications was not consistent, and that A1c variability representing long term glucose fluctuation may be related to coronary atherosclerosis in patients with type 1 diabetes. In this study, we attempt to determine whether or not A1c variability can predict coronary artery disease (CAD) in patients with type 2 diabetes.
Methods We reviewed data of patients with type 2 diabetes who had undergone coronary angiography (CAG) and had been followed up with for 5 years. The intrapersonal standard deviation (SD) of serially-measured A1c levels adjusted by the different number of assessments among patients (adj-A1c-SD) was considered to be a measure of the variability of A1c.
Results Among the 269 patients, 121 of them had type 2 diabetes with CAD. In patients with A1c ≥7%, the mean A1c levels and A1c levels at the time of CAG among the three groups were significantly different. The ratio of patients with CAD was the highest in the high adj-A1c-SD group and the lowest in the low adj-A1c-SD group (
P =0.017). In multiple regression analysis, adj-A1c-SD was an independent predictor for CAD in subjects with A1c ≥7% (odds ratio, 2.140;P =0.036).Conclusion Patients with higher A1c variability for several years showed higher mean A1c levels. A1c variability can be an independent predictor for CAD as seen in angiographs of patients with type 2 diabetes with mean A1c levels over 7%.
-
Citations
Citations to this article as recorded by- Intermediate- and long-term associations between air pollution and ambient temperature and glycated hemoglobin levels in women of child bearing age
Mike Z. He, Itai Kloog, Allan C. Just, Iván Gutiérrez-Avila, Elena Colicino, Martha M. Téllez-Rojo, María Luisa Pizano-Zárate, Marcela Tamayo-Ortiz, Alejandra Cantoral, Diana C. Soria-Contreras, Andrea A. Baccarelli, Robert O. Wright, Maayan Yitshak-Sade
Environment International.2022; 165: 107298. CrossRef - Correlation between HbA1c and Triglyceride Level with Coronary Stenosis Degree in Type 2 Diabetes Mellitus with Coronary Heart Disease
Laily Adninta, Indranila Samsuria, Edward Kurnia Setiawan Limijadi
Open Access Macedonian Journal of Medical Sciences.2022; 10(B): 944. CrossRef - Long-Term Glycemic Variability and Vascular Complications in Type 2 Diabetes: Post Hoc Analysis of the FIELD Study
Emma S Scott, Andrzej S Januszewski, Rachel O’Connell, Gregory Fulcher, Russell Scott, Antero Kesaniemi, Linda Wu, Stephen Colagiuri, Anthony Keech, Alicia J Jenkins
The Journal of Clinical Endocrinology & Metabolism.2020; 105(10): e3638. CrossRef - How Continuity in Service Impacts Process Variability: Evidence from a Primary Care Setting
Vishal Ahuja, Carlos Alvarez, Bradley R. Staats
SSRN Electronic Journal .2019;[Epub] CrossRef - Association of hemoglobin A1c variability and the incidence of heart failure with preserved ejection fraction in patients with type 2 diabetes mellitus and arterial hypertension
Jun Gu, Yu-Qi Fan, Jun-Feng Zhang, Chang-Qian Wang
Hellenic Journal of Cardiology.2018; 59(2): 91. CrossRef - Prognostic impact of HbA1c variability on long-term outcomes in patients with heart failure and type 2 diabetes mellitus
Jun Gu, Jian-an Pan, Yu-qi Fan, Hui-li Zhang, Jun-feng Zhang, Chang-qian Wang
Cardiovascular Diabetology.2018;[Epub] CrossRef - Cardiovascular Autonomic Neuropathy Predicts Higher HbA1c Variability in Subjects with Type 2 Diabetes Mellitus
Yeoree Yang, Eun-Young Lee, Jae-Hyoung Cho, Yong-Moon Park, Seung-Hyun Ko, Kun-Ho Yoon, Moo-Il Kang, Bong-Yun Cha, Seung-Hwan Lee
Diabetes & Metabolism Journal.2018; 42(6): 496. CrossRef - Glycated hemoglobin level is an independent predictor of major adverse cardiac events after nonfatal acute myocardial infarction in nondiabetic patients
Chin-Lan Chen, David H.-T. Yen, Chin-Sheng Lin, Shih-Hung Tsai, Sy-Jou Chen, Wayne H.-H. Sheu, Chin-Wang Hsu
Medicine.2017; 96(18): e6743. CrossRef - Randomized, Open-Label, Parallel Group Study to Evaluate the Effect of Internet-Based Glucose Management System on Subjects with Diabetes in China
Hun-Sung Kim, Chenglin Sun, So Jung Yang, Lin Sun, Fei Li, In Young Choi, Jae-Hyoung Cho, Guixia Wang, Kun-Ho Yoon
Telemedicine and e-Health.2016; 22(8): 666. CrossRef - Association between hemoglobin A1c variability and subclinical coronary atherosclerosis in subjects with type 2 diabetes
Hae Kyung Yang, Borami Kang, Seung-Hwan Lee, Kun-Ho Yoon, Byung-Hee Hwang, Kiyuk Chang, Kyungdo Han, Gunseog Kang, Jae Hyoung Cho
Journal of Diabetes and its Complications.2015; 29(6): 776. CrossRef - Glycated Albumin Levels in Patients with Type 2 Diabetes Increase Relative to HbA1cwith Time
Hye-jin Yoon, Yong-ho Lee, Kwang Joon Kim, So Ra Kim, Eun Seok Kang, Bong-Soo Cha, Hyun Chul Lee, Byung-Wan Lee
BioMed Research International.2015; 2015: 1. CrossRef - Brief Review of Articles in 'Endocrinology and Metabolism' in 2013
Won-Young Lee
Endocrinology and Metabolism.2014; 29(3): 251. CrossRef - Inverse Association between Glycated Albumin and Insulin Secretory Function May Explain Higher Levels of Glycated Albumin in Subjects with Longer Duration of Diabetes
Yong-ho Lee, Mi Hyang Kown, Kwang Joon Kim, Eun Young Lee, Daham Kim, Byung-Wan Lee, Eun Seok Kang, Bong Soo Cha, Hyun Chul Lee, Marià Alemany
PLoS ONE.2014; 9(9): e108772. CrossRef - HbA1c Variability and Micro- and Macrovascular Complications of Diabetes
Hae Kyung Yang, Seung-Hwan Lee
The Journal of Korean Diabetes.2014; 15(4): 202. CrossRef - Letter: A1c Variability Can Predict Coronary Artery Disease in Patients with Type 2 Diabetes with Mean A1c Level Greater than 7 (Endocrinol Metab 2013;28:125-32, Eun Ju Lee et al.)
Hye Seung Jung
Endocrinology and Metabolism.2013; 28(4): 346. CrossRef
- Intermediate- and long-term associations between air pollution and ambient temperature and glycated hemoglobin levels in women of child bearing age


 KES
KES

 First
First Prev
Prev



